–
If standard doses of nitrate – NTG (NiTroGlycerin – GTN GlycerylTriNitrate in Commonwealth countries), ISDN (IsoSorbide DiNitrate), or ISMN (IsoSorbide MonoNitrate) improve outcomes for CHF/ADHF (Congestive Heart Failure/Acute Decompensated Heart Failure) patients, and larger IV (IntraVenous) doses are more effective than standard doses,[1],[2],[3],[4],[5],[6],[7],[8],[9],[10],[11],[12] what method(s) of drug delivery works best?
High dose IV drip?
High dose IV bolus?
A high dose IV bolus combined with a high dose IV drip?
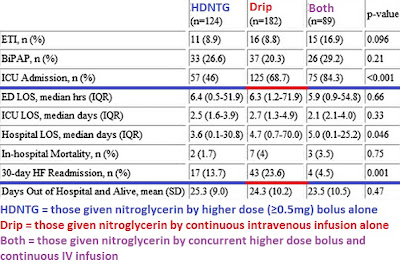
We performed a retrospective cohort study of patients who presented to the emergency department (ED) of an urban, teaching hospital with severe, acute hypertensive heart failure between Jan 2007 and July 2011 and received intravenous nitroglycerin. 3 subgroups were defined: 1) those given nitroglycerin by higher dose (≥ 0.5 mg) bolus alone (higher dose nitroglycerin); 2) those given nitroglycerin by continuous intravenous infusion alone (intravenous nitroglycerin); and 3) those given nitroglycerin by concurrent higher dose bolus and continuous IV infusion (higher dose intravenous nitroglycerin).[13]
At least half a milligram at a time means at least 25% more than the standard bolus dose with a NTG tab/spray.
Click on images to make them larger.
With bolus dosing the blood pressure dropped more quickly.
The sooner we drop the patient’s blood pressure, as long as we do not drop it too much, the better for the patient.
Do we really have a problem with dropping the pressure too much with high doses of bolus IV NTG?
No.
Almost every severely hypotensive patient in this study received more than 1 mg/minute IV NTG, which would be boluses of at least 5 mg IV NTG every 5 minutes until they improved – and most did improve dramatically.[14]
Conclusion: In this single-center, retrospective, unadjusted analysis of primarily African-American patients with acute hypertensive heart failure, nitroglycerin administered by higher dose bolus without concurrent intravenous infusion was associated with a significant decrease in ICU admissions and hospital length of stay. Based on our findings, bolus higher dose nitroglycerin appears to be a viable option for the management of such patients.[13]
There are some important questions about IV bolus dosing of NTG for CHF/ADHF.
How aggressive should our initial bolus dose be?
How often should we repeat the dosing?
NTG is metabolized very quickly, so these boluses are only to treat the initial emergency, then the patient will be switched to an infusion of NTG.
We do need more research, but we also need research that does not include furosemide, or compares furosemide with a placebo.
This evidence is much better than any evidence used to justify epinephrine in cardiac arrest. If any CHF/ADHF patients have a cardiac arrest and they are not immediately resuscitated, they are supposed to be treated with epinephrine according to the current ACLS (Advanced Cardiac Life Support) guidelines.
These patients do not arrest due to any deficiency of adrenaline (epinephrine).
These patients improve with treatment that is essentially the opposite of epinephrine.
–
Footnotes:
–
[1] [The efficacy of isosorbide dinitrate administered in an intravenous bolus in acute cardiogenic pulmonary edema].
Rabaçal C, Ribeiro H, Nuno L, Mendonça C, Linder J, Pereira D, Carvalho E, Afonso JS, Fernandes JS.
Rev Port Cardiol. 1993 Dec;12(12):1029-35, 1000. Portuguese.
PMID: 8117456 [PubMed – indexed for MEDLINE]
–
[2] Intravenous nitroglycerin boluses in treating patients with cardiogenic pulmonary edema.
Nashed AH, Allegra JR.
Am J Emerg Med. 1995 Sep;13(5):612-3. No abstract available.
PMID: 7662071 [PubMed – indexed for MEDLINE]
–
[3] Intravenous nitrates in the prehospital management of acute pulmonary edema.
Bertini G, Giglioli C, Biggeri A, Margheri M, Simonetti I, Sica ML, Russo L, Gensini G.
Ann Emerg Med. 1997 Oct;30(4):493-9.
PMID: 9326864 [PubMed – indexed for MEDLINE]
–
[4] Randomised trial of high-dose isosorbide dinitrate plus low-dose furosemide versus high-dose furosemide plus low-dose isosorbide dinitrate in severe pulmonary oedema.
Cotter G, Metzkor E, Kaluski E, Faigenberg Z, Miller R, Simovitz A, Shaham O, Marghitay D, Koren M, Blatt A, Moshkovitz Y, Zaidenstein R, Golik A.
Lancet. 1998 Feb 7;351(9100):389-93.
PMID: 9482291 [PubMed – indexed for MEDLINE]
–
[5] High-dose intravenous isosorbide-dinitrate is safer and better than Bi-PAP ventilation combined with conventional treatment for severe pulmonary edema.
Sharon A, Shpirer I, Kaluski E, Moshkovitz Y, Milovanov O, Polak R, Blatt A, Simovitz A, Shaham O, Faigenberg Z, Metzger M, Stav D, Yogev R, Golik A, Krakover R, Vered Z, Cotter G.
J Am Coll Cardiol. 2000 Sep;36(3):832-7.
PMID: 10987607 [PubMed – indexed for MEDLINE]
Free Full Text and Free PDF Download from ScienceDirect
–
[6] Administering a glyceryl trinitrate infusion: big is not always best.
Reed MJ.
Emerg Med J. 2007 Jun;24(6):423-4.
PMID: 17513541 [PubMed – indexed for MEDLINE]
Free Full Text from PubMed Central
–
[7] Administering a glyceryl trinitrate infusion: faster is better than slower.
Steel A, Varley J.
Emerg Med J. 2008 Jan;25(1):60. No abstract available.
PMID: 18156558 [PubMed – indexed for MEDLINE]
–
[8] Treatment of severe decompensated heart failure with high-dose intravenous nitroglycerin: a feasibility and outcome analysis.
Levy P, Compton S, Welch R, Delgado G, Jennett A, Penugonda N, Dunne R, Zalenski R.
Ann Emerg Med. 2007 Aug;50(2):144-52. Epub 2007 May 23.
PMID: 17509731 [PubMed – indexed for MEDLINE]
Free Full Text PDF Download from Ferne.org
–
[9] High dose nitroglycerin treatment in a patient with cardiac arrest: a case report.
Guglin M, Postler G.
J Med Case Reports. 2009 Aug 10;3:8782.
PMID: 19830240 [PubMed]
Free Full Text from PubMed Central
–
[10] A Protocol of Bolus-Dose Nitroglycerin and Non-Invasive Ventilation to Avert Intubation in Emergency Department Acute Pulmonary Edema
Piyush Mallick, Surjya Upadhyay, TS Senthilnathan, El Matit Waleed , Al Jahra Hospital, Scott Weingart, Mount Sinai School of Medicine
Prepublication abstract
PDF Download of page at EMCrit
–
[11] EMCrit Podcast 1-Sympathetic Crashing Acute Pulmonary Edema
by EMCRIT on April 25, 2009
Link to Podcast page
Link to page with other evidence supporting this treatment
–
[12] Isosorbide dinitrate bolus for heart failure in elderly emergency patients: a retrospective study.
Freund Y, Delerme S, Boddaert J, Baker E, Riou B, Ray P.
Eur J Emerg Med. 2011 Oct;18(5):272-5.
PMID: 21499108 [PubMed – indexed for MEDLINE]
–
[13] Nitroglycerin for Treatment of Acute, Hypertensive Heart Failure: Bolus, Drip or Both?
Kwiatkowski GM, Saely S, Purakal J, Mahajan A, Levy PD/Detroit Receiving Hospital, Detroit, MI; Wayne State University School of Medicine, Detroit, MI
Annals of Emergency Medicine, Volume 60, issue 4 (October, 2012), p. S9.
ISSN: 0196-0644 DOI: 10.1016/j.annemergmed.2012.06.049
Abstract 22 Indexed with OhioLINK Journal Article Locator
–
[14] What is the basis for post-resuscitation treatment recommendations?
Rogue Medic
Mon, 15 Oct 2012
Article
–
Kwiatkowski, G.M.; Saely, S.; Purakal, J.; Mahajan, A.; Levy, P.D. (2012). Nitroglycerin for Treatment of Acute, Hypertensive Heart Failure – Bolus, Drip or Both? Annals of Emergency Medicine, 60 (4), 59-59
.



With our protocols of sublingual q 3-5 min until CPAP and drip of 50-200 mcg we are effectively doing a bolus prior to high dose. Had very good outcomes with it.
I think everything said was actually very reasonable.
But, what about this? what if you composed a catchier title?
I mean, I don’t want to tell you how to run your website, however what if you added a headline that grabbed people’s attention?
I mean Nitroglycerin for Treatment of Acute, Hypertensive
Heart Failure – Bolus, Drip or Both? | Rogue Medic is a little vanilla.
You should peek at Yahoo’s front page and note how they create news titles to get people to click. You might add a related video or a picture or two to get people excited about what you’ve got to say.
Just my opinion, it could make your posts a little bit more interesting.