In the comments to No More Comments on Popular Science is this from Duke Powell –
Rogue Medic says Epinephrine is no good.
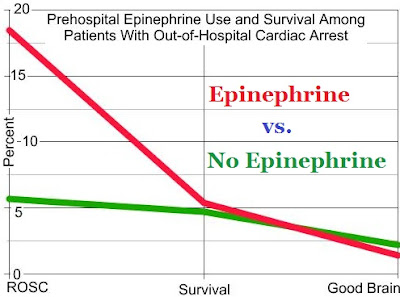
I have been critical of epinephrine because we are routinely giving epinephrine in cardiac arrest, but we do not have any evidence that epinephrine improves any outcome that matters. ROSC (Return Of Spontaneous Circulation) is not an outcome that matters. Epinephrine does improve ROSC, but there is no increase in people leaving the hospital with good brain function (the outcome that matters and surviving for more time is better). There is evidence of harm.[1] The evidence of harm is not great, but the evidence of benefit does not exist.
More ROSC, but fewer survivors. That is not a benefit.
I do not claim that epinephrine is good, bad, or neutral. I point out that there is probably a subset of cardiac arrest patients who do benefit from epinephrine, but we have no way of knowing who those patients are.
I describe the lack of evidence of benefit and explain that standards of care should be supported by valid evidence of improved outcomes.
He says backboards are no good.
There is also no valid evidence of improved outcomes with backboards for unstable spinal fractures.
Where is the evidence that using backboards on patients with unstable spinal fractures results in fewer disabled patients (the outcome that matters)? There is evidence of harm.[2] The evidence of harm is not great, but the evidence of benefit does not exist.
Rogue Medic disagrees about a lot of things that scientists have said are “best practices” for EMS.
Scientists?
What scientists?
I disagree with using treatments that are not based on valid science.
I disagree even more strongly with standards of care that are not based on valid science.
I am also very critical of bad science, even if the results agree with what I think is true.[3],[4]
In most instances this medic with over 40 years experience agrees with Mr Rogue Medic. Not because of the science, but because of my experience.
That is not a very good reason for disagreeing with standards of care. It is a good reason for asking questions of the people who would know about the evidence, but even a 40 year career is just a series of anecdotal experiences. What kind of control has been used to minimize the effects of bias?
What has been done to make sure that confirmation bias does not limit recollection to those anecdotes that support individual bias?
But disagree with him on global warming? He calls you a science denier and says you can’t think for yourself.
I described some of the reasons you appear to be a science denialist above. That is science denialism on the topic of EMS.
You would get the same responses to EMS science denialism if you understood climate change. There are people who are willing to agree with science when it agrees with their prejudices, but are science denialists when science does not confirm their prejudices.
The problem is with the people, not with science.
Science does not care about prejudices.
Science just tells us what is real.
Science is not perfect.
Because science is not perfect, it depends on confirmation by different methods and by replication (preferably more than once). And most of all, science depends on rigorous attempts at objectivity, because everyone has biases.
Science does not exist to confirm biases.
Fact of the matter is, I am thinking for myself in terms of climate change. I’m not the guy following the crowd. Just as you are not the guy following the crowd with EMS best practice.
I am the guy basing decisions on science.
You appear to be the guy claiming that science does not matter. You appear to be the guy basing decisions on politics.
It isn’t the decision that matters, but the way we get there. Political decisions should be made based on valid science, rather than denying science or trying to make science fit political goals.
BTW, make sure your furnace is working, things are about to get colder, starting tomorrow.
Ha!!
Now you are discussing weather.
You do not appear to know the difference between weather and climate, but you seem to think that you know enough to tell scientists that they are wrong.
Thank you for reinforcing my point.
–
Footnotes:
–
[1] Prehospital epinephrine use and survival among patients with out-of-hospital cardiac arrest.
Hagihara A, Hasegawa M, Abe T, Nagata T, Wakata Y, Miyazaki S.
JAMA. 2012 Mar 21;307(11):1161-8. doi: 10.1001/jama.2012.294.
PMID: 22436956 [PubMed – indexed for MEDLINE]
–
[2] Out-of-hospital spinal immobilization: its effect on neurologic injury.
Hauswald M, Ong G, Tandberg D, Omar Z.
Acad Emerg Med. 1998 Mar;5(3):214-9.
PMID: 9523928 [PubMed – indexed for MEDLINE]
Free Full Text from Academic Emergency Medicine.
–
[3] Prehospital Intravenous Fluid Administration is Associated With Higher Mortality in Trauma Patients – Part I, Part II, and Part III
Rogue Medic
02/20/2011
Part I
02/22/2011
Part II
03/01/2011
Part III
–
[4] Prehospital Intravenous Fluid Administration is Associated With Higher Mortality in Trauma Patients: A National Trauma Data Bank Analysis.
Haut ER, Kalish BT, Cotton BA, Efron DT, Haider AH, Stevens KA, Kieninger AN, Cornwell EE 3rd, Chang DC.
Ann Surg. 2010 Dec 20. [Epub ahead of print]
PMID: 21178760 [PubMed – as supplied by publisher]
Full Text in PDF format from www.medicalscg
.



RM,
The climate issue has historically been too politically charged (by both the left and right) to make any headway with an individual who, by late 2013, does not accept that average global temperature is increasing along with associated phenomena like wild fires, droughts, shoreline recession, flooding, etc. Frankly, I think the left is mostly to blame; accepting that pollution has environmental consequences would be straightforward enough for most (after all, China is the #1 CO2 emitter), but the left went further than that, integrating it into their tired old Gaianism shtick. That the well-being of the (quote)Earth(/unquote) comes before the well-being of humans.
Rather than acknowledging the reality that hydrocarbons are the vital lifeblood of modern civilization, that they are the ultimate root of the existence of billions of additional people who otherwise could not have been sustained in a pre-industrial world without the technologies fueled (literally) by hydrocarbons; rather than acknowledge that *even the most dire consequences of climate change* cannot even remotely approach the good that hydrocarbons have done and are doing, and the inescapable reality *no matter what alternatives are available, our civilization *WILL* run on hydrocarbons, and we *WILL* exhaust all hydrocarbons of prehistoric origin.
The effects of climate change and depletion of fossil fuels (the time table for which has been greatly exaggerated) are alone enough to spur response; indeed, the flood of refugees from areas like Bangladesh and Tunisia (which will likely be the first major victims of climate-related catastrophes), the abandonment of places like the Maldives, the rising price of fossil fuels as extraction becomes increasingly expensive, all of these will generate responses without banner-waving or passionate pleas to establish new hippie communes.
The insurance industry has already shifted its focus to climate change, as have leaders of various businesses across the world. An increasing number of “everyday people” “on the ground,” who aren’t myopic but just don’t have the time to see the big picture away from their own day-to-day concerns, will be confronted with an increasing number of catastrophes that will touch their lives in various ways. People in the southwestern US or Australia won’t care about arguing that something does or doesn’t “exist” when more and more of their communities are ravaged by epic wild fires of historic proportions. People who live on coastlines won’t give a crap about going “green” or whether climate change is a leftwing “conspiracy” when the homes they’ve rebuilt are destroyed yet again by storm surge and beach erosion.
This is already too long, but my point is that if the left hadn’t turned this into a crusade to demonize and abandon fossil fuels, or made it synonymous with their “mother earth > humans” philosophy, I feel nobody would be arguing about whether or not something obviously real that’s obviously a problem is in fact real.
That said, even though people will get hurt, even though climate change is a problem, it’s not as big a deal as the left makes it out to be. We’ve been through much, much, much worse (e.g. black death). And there are far more dangerous threats we’ll face in this century (e.g. human-engineered viruses/bioterrorism for one).
FWIW, I agree with you, I only think the issue is not exactly as it seems.
BTW:
As someone pursuing an MD-PhD with a focus on emergency medicine, I love this quote:
“ROSC (Return Of Spontaneous Circulation) is not an outcome that matters.”
It’s incredible that many people in emergency medicine don’t even appreciate this fact.
– T.L.
Taurus,
That may be the case. It has been going on so long, we could trace it well beyond the Luddites, that it does not matter what started the denial of science.
I do not care about the politics. I have no fondness for the science denialism of the left, which is also a huge problem.
I write about topics that have a topic that catches my eye and that continues to interest me as I look at it in more depth.
–
An understanding of the difference between disease-oriented outcomes (such as ROSC, or lowering the blood pressure by 5 points, or eliminating ventricular ectopy, . . . ) and patient-oriented outcomes (such as survival, or a cure of the disease, . . . ) is something that eludes many people.
Are we supposed to be doing what is best for the surrogate endpoint (disease-oriented outcome) or are we supposed to be doing what is best for the patient (patient-oriented outcome)?
Everyone will recognize that the patient is what matters, but many find excuses for changing the goals to disease-oriented outcomes after becoming frustrated with the difficulty of improving outcomes that matter.
Gosh! That is so hard. I think I need to lower my standards, so that I can achieve success.
I see things improving, but I also see a lot of resistance from people who manage to convince themselves that surrogate endpoints matter to real patients.
A similar problem is with testing. The result of a test does not justify a test. We have a very poor understanding of the importance of prior probability in interpreting the results of tests. What is the false positive rate? What is the false negative rate? If we consider these, many test results take on entirely different meanings.
I used to think that one big problem was pain management, but now I think is more of a symptom of not understanding the actual risks and benefits for each patient.
.