In response to Dextrose 10% or 50% in the treatment of hypoglycaemia out of hospital? A randomised controlled trial. There is this comment from Can’t say, clowns will eat me –
Ok, I’ve seen this study many times and even referenced it to many people at differing levels of providership. That being said one of the most interesting arguments I’ve heard is that basically the people saying this thought, their blood sugar is critically low and they’re killing brain cells and if we don’t push D50 and push it as fast as possible we’re going to essentially cause a brain injury.
There is no reason to believe that there is any harm to the patient with 10% dextrose.
That brain damage assumes that it takes longer for the patient to be treated with 10% dextrose than with 50% dextrose.
The average time to return to full consciousness with 50% dextrose?
8 minutes.
The average time to return to full consciousness with 10% dextrose?
8 minutes.
Where is the difference?
Maybe the people making these excuses are the ones with brain damage causing them to see a big difference between 8 minutes and 8 minutes, but those of us without brain damage realize that time does not speed up or slow down depending on the concentration of dextrose.
The brain damage is more likely just operator error. The operator error is bias. The people are biased against something they are not familiar with. This leads them to assume that there are problems with the unfamiliar, even though these problems do not exist.
–
Also, I’ve heard the argument as to the previous post about the administration guidelines of the approximately 30 minutes it’d take to push it being too long
There is no 30 minutes.
30 minutes is a lie from the biased opponents of better patient care.
–
. . . as above but also that tied in with the D10 drip to stop rebound hypoglycemia just not being “practical” because we can’t spend that long with the patient, etc. Why is that wrong? Is it better to cause tissue necrosis? rebound hypoglycemia and by their own logic, even further brain damage?
There were differences in scene times between the 10% dextrose and the 50% dextrose groups, but that is to be expected with any new and unfamiliar method of treatment. In this study, a 3 way stopcock was used to draw 10% dextrose from the IV bag into a syringe, then switch the direction of flow to the patient and push the 10% dextrose that had been drawn into the syringe. This is more complicated than the method of giving 50% dextrose, but there are many other ways to give 10% dextrose.
The difference in time was only in the total scene time, not in the treatment time.
The fastest scene times and the fastest recovery times were in the 10% dextrose group.
This raises questions about the skills of the people who claim that we cannot give an adequate amount of 10% dextrose in less than 30 minutes –
How drunk and stupid are they?
But they aren’t necessarily drunk, or even stupid. What they are is biased.
Biased people aren’t necessarily bad people, but they are dangerous.
What else do we call refusing to provide better care to our patients just because of bias?
A refusal to provide better care is a demand to provide worse care. This is dangerous.
–
If this were a National Registry of EMTs testing station, nobody would have any problem with whatever 10% dextrose administration method was being tested, because we would practice until they were able to do it consistently and quickly.
If we cannot consistently wake up hypoglycemic patients with 10% dextrose in the same amount of time as with 50% dextrose, maybe we should not be allowed to use dopamine or lidocaine or amiodarone drips.
Clearly a drip set is more than a little bit beyond our capabilities as paramedics.
And if we can’t manage a simple IV drip set, we certainly can’t manage an endotracheal tube. 😳
Perhaps we do not want to use that argument.
–
Why not just come in and establish a line and administer D10 via a drip. And, the administrators will love this. You won’t be tied up on scene unavailable, you won’t be unavailable going to the hospital after the call without a patient(in which case you oftentimes will be paid little or nothing) and you’ll transport more and make more money for the company. For those in the private sector, wouldn’t that be a boon to reimbursements?
I don’t see any need to change transport for a difference in recovery time that is zero minutes.
There is no important difference in treatment time.
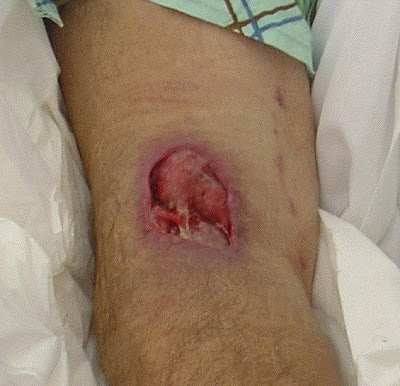
There is a dramatic difference in the potential for bad outcome with the unnecessary high concentration of the 50% dextrose.
Does a surgeon require the greater risk of general anesthesia for something that can be treated under local anesthesia?
Do we fly every patient?
Do we drive everywhere with lights and sirens?
We consider the benefits and risks of treatments.
We use the treatment that provides adequate benefit without unnecessary risk.
50% dextrose provides a greater risk for no greater benefit.
–
The picture is one I found labeled as being from Annals of Emergency Medicine of 50% Dextrose extravasation, but I do not know anything about which issue it is from or any other details – update – the image credit is below.
Images in emergency medicine. Dextrose extravasation causing skin necrosis.
Levy SB, Rosh AJ.
Ann Emerg Med. 2006 Sep;48(3):236, 239. Epub 2006 Feb 17. No abstract available.
PMID: 16934641 [PubMed – indexed for MEDLINE]
.
.jpg)


Subscribe to RogueMedic.com