–
Dr. Radecki at EM Literature of Note has a nice analysis of a study that promises to try to change medicine for the worse. Of course, that is not the intent of the study’s authors, but they have too much confidence in their results. The study is only looking at patients with minor head injury and minor symptoms, but taking warfarin (Coumadin).
–
Patient flow is shown in the Figure, with 97 patients observed according to our protocol. Ten of these patients declined the second CT scan; all remained asymptomatic and none were readmitted within 30 days because of symptoms related to the head injury.[1]
These 10 patients – patients with no signs of any complications for 30 days – were excluded because they did not complete the protocol.
I admire the authors’ attempts at adherence to their protocol, but there is a problem with their placing more emphasis on a flawed protocol, than they place on the patient outcomes.
Was the purpose of the study to evaluate the ability of the protocol to predict something?
Outcome Measures
Two investigators (V.G.M. and M.L.) reviewed the electronic medical record (Sistema Informatico Ospedaliero, Fly Tecnologie e Servizi, Perugia, Italy) to identify the presence or absence of the following outcomes: acute traumatic intracranial lesion (defined earlier) on the second CT scan, death, admission for any CT abnormality, operative neurosurgery, or readmission within 30 days because of symptoms related to the head injury.[1]
The ability of a second CT scan to identify problems was only one of the outcomes being measured. The authors should not have excluded these 10 patients from the other outcomes.
–
–
How do we come up with 6% bad outcomes?
It all depends on how we define our outcomes.
Is there a big difference between 1/87 having neurosurgery and 1/97 having neurosurgery?
Not really, but it does allow the authors to turn 5/97 (5%) into 5/87 and it becomes 6%. The bigger the number, the more significant impressive the result. This would suggest that their 24 hour observation period for minor head injury is a good idea, but how good was their protocol at identifying admission for signs of intracranial bleeding?
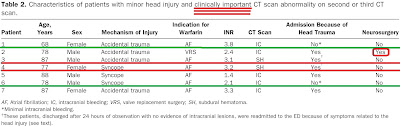
Two additional patients (2%; 95% CI 0.5% to 5%) who were discharged after a negative second CT scan result were readmitted 2 and 8 days later, one with confusion and the second with headache. Their initial presentations were accidental trauma and syncope, respectively; however, both had an initial international normalized ratio of greater than 3.0 (Table 2). Both had subdural hematomas without mass effect; neither required neurosurgery (Table 2).[1]
We will look at Table 2, but first let’s look at Table 3 –
–
–
I already provided you with a quote that contradicts what is shown in Table 3.
It is true that 5/7 is 71%, but . . .
the second CT was negative for 2 of these patients. It was only after the two patients returned complaining of symptoms suggestive of head injury that each had a third CT scan.
–
–
The correct calculation would be quite a bit different.
Out of 87 patients, 5 patients had positive second CTs, but 2 were discharged because the bleeding was not considered significant.
3/5 were admitted based on a second CT.
The math is easy on that one – 60% – not 71%.
Of the patients admitted for head injury, 2 had negative second CT scans and only had third CT scans because of symptoms that caused the patients to return to the hospital.
In other words 2/82 had false negative second CT scans – if admission is the criterion being examined. 82 because we cannot include the 10 who refused a second CT, nor can we include the 5 who had positive CT scans.
How useful is this protocol?
2 patients with positive CTs discharged with no sequelae.
2 patients with positive CTs admitted with no sequelae.
1 patient with positive CT admitted and treated with neurosurgery.
2 patients with negative CTs discharged, but returned with sequelae and admitted.
Is the 24 hour observation and second CT scan able to predict admission?
After the second CT scan, only 60% were admitted, but 60% is just barely better than flipping a coin. that might be worth paying attention to, but they only found 60% of total admissions by this method.
The protocol completely missed 40% of the total admissions. These patients stayed for 24 hours of observation; these patients agreed to the second CT scan; these patients had negative second CT scans; these patients were discharged after completely following the protocol and having no positive findings. These patients returned with symptoms of head injuries.
One patient returned after 2 days and the other patient returned after 8 days. Neither patient ended up having neurosurgery.
Accordingly, our findings support both the advisability of initial CT scanning and the 24-hour observation and repeated CT protocol advocated by the European guidelines.4 [1]
Absolutely not.
However, because both of our patients with delayed hemorrhage had an initial international normalized ratio of greater than 3.0, longer observation may be warranted in this subset.[1]
Maybe.
Maybe not.
What kind of treatment did these patients receive?
Nothing is specified in the paper. They might have received medication. they might just have been observed. We do not know.
The only patient who ended up having neurosurgery had an INR of 2.4. Although 8 of the 87 patients receiving a second CT scan had INRs over 3, we do not know how many of the patients, who were admitted, but refused the second CT scan might have had INRs over 3.
How many of the neurosurgery patients had an INR of over 3?
Zero.
–
Is the 24 hour observation and second CT scan able to predict neurosurgery?
Maybe.
Maybe not.
The most important flaw in this study is presuming that we can use fewer than 100 patients to identify the incidence of a rare condition.
We need to expect that the number of patients studied will not be representative, when the incidence of what is being studied is so uncommon. When each patient makes up more than 1 percent of the total and the total number of patients having surgery is just one, how can we conclude that we are learning anything from the research.
This is an example of research that is only going to confirm biases.
Confirmation of biases is not the purpose of research.
–
Supervising editor: Steven M. Green, MD[1]
With all of his experience, Dr. Green should know better than to accept this.
–
However, we simply cannot expose all anticoagulated patients with minor head trauma to the harms and costs of hospitalization. Better studies are required to prospectively determine the risk profile of patients who require further observation in a hospital setting, rather than a watchful discharge home.[2]
Absolutely.
Go read Dr. Radecki’s analysis and especially the comment of steve, who might need to get his own blog. 🙂
–
Footnotes:
–
[1] Management of Minor Head Injury in Patients Receiving Oral Anticoagulant Therapy: A Prospective Study of a 24-Hour Observation Protocol.
Menditto VG, Lucci M, Polonara S, Pomponio G, Gabrielli A.
Ann Emerg Med. 2012 Jan 13. [Epub ahead of print]
PMID: 22244878 [PubMed – as supplied by publisher]
Free Full Text from Annals of Emergency Medicine
–
[2] Observation For Anticoagulated Head Trauma
EM Literature of Note
Radecki
Article
–
Menditto, V., Lucci, M., Polonara, S., Pomponio, G., & Gabrielli, A. (2012). Management of Minor Head Injury in Patients Receiving Oral Anticoagulant Therapy: A Prospective Study of a 24-Hour Observation Protocol Annals of Emergency Medicine DOI: 10.1016/j.annemergmed.2011.12.003
.




[…] Medic gives an illustrated example on how bad medicine gets practiced by good […]