.jpg)
Also posted over at Paramedicine 101. Go check out the rest of what is there.
CAST (The Cardiac Arrhythmia Suppression Trial)[1] was a large scale randomized placebo controlled trial. This was to determine which of the antiarrhythmics would be able to claim the title as the most effective life saving drug on the planet. CAST was one of the most important EMS studies ever done. And CAST wasn’t even an EMS study.
Moricizine vs. encainide vs. flecainide to see what saves the most lives.
Which drug won?
We’re not there, yet.
The experts understood the pathophysiology. They knew how to fix it.
What did the experts see as the problem, pathophysiologically?
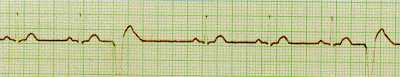
After a heart attack, many people will have some extra heart beats. Beats apparently originating in the part of the heart damaged by the heart attack. These are most commonly called PVCs (Premature Ventricular Contractions). 2 PVCs are circled in red below. They are also called VPBs (Ventricular Premature Beats) or even FLBs (Funny Looking Beats), but most commonly PVCs.
After a heart attack (MI or Myocardial Infarction), people with plenty of PVCs (post-MI PVCs) will experience SCA (Sudden Cardiac Arrest) at a higher rate than other people who have had heart attacks, but do not have post-MI PVCs.
That much is accepted. In extrapolating from this. They concluded that if patients with frequent post-MI PVCs were more likely to have SCA, they could prevent SCA by preventing the post-MI PVCs.
Sounds reasonable.
It is reasonable. The problem is that they never tested the theory on a large enough group of people, until CAST, to demonstrate how well the theory worked. At the time, these drugs became the top selling drugs. Sales-wise, they were the Prozac and Viagra of the time. They were a hugely profitable part of the drug market. Yet there was no evidence that they saved lives. Only theory. Only pathophysiology. CAST was designed to show how good they were at saving lives.
Preventing post-MI PVCs is pretty easy. Improving survival is a little more complicated.
Why did people accept that fewer post-MI PVCs is the same as improving survival?
The top electrophysiologists were in agreement about how the heart works. Based on their research showing higher mortality with frequent post-MI PVCs, they told people that this was the best way to save lives.
After a patient had a heart attack, they would record an ECG that showed post-MI PVCs, such as the ECG below.
Then they would give patients the medication. As the medication began to work, the post-MI PVCs went away.
Obviously much better. This is proof that the heart is better and the patient is healthier.
Actually, if the ECG is the face that the heart shows us, this is just a form of Botox for the face of the ECG. We are making it look as it did before the heart attack. Remember, this was just for patients who had a heart attack – post-MI PVCs. The problem is that the antiarrhythmic medications interfere with the conduction system to make the post-MI PVCs disappear. The result of that tinkering is not limited to making the PVCs go away. Some of the other effects are still unclear.
The results of earlier studies were clear that the antiarrhythmic medications made the post-MI PVCs go away. This was viewed as a success. This was only a success at treating a surrogate end point. A surrogate end point is often studied, because it does not require as large a study group as an experiment that is set up to show a difference in meaningful outcome.
What is meaningful outcome?
Survival with a good quality of life.
When we look at all of the drugs that are used in cardiac arrest, we are looking at drugs that have been shown to be effective, at least a little bit, but only at improving surrogate end points. Surrogate end points are appropriate for initial studies, but with widespread use of a treatment, we need to look at meaningful outcomes.
In cardiac arrest, epinephrine is great at getting a heart to beat again (ROSC, or Return Of Spontaneous Circulation). Unfortunately, getting a pulse back, but dying in the hospital, is not a good outcome.[2] Having the heart rate go from zero to 200 may not not be the best way to calm down a heart that has just experienced SCA, possibly due to overstimulus. This is one of the reasons for the introduction of vasopressin. Vasopressin is less of a stimulant to the heart, less of a cocaine-like jolt to the heart.
In EMS we used to give nifedipine in hypertensive crisis,[3] because it lowered the blood pressure. It really lowered the blood pressure. The problem was that we were treating a surrogate end point.
Oxygen[4] is another treatment that many of us give just because of surrogate end points. We seem to be trying to get 110% out of the SpO2, rather than treat the patient. We have not done enough research to know when oxygen is harmful. Hypothermic resuscitation is believed to work by preventing post-resuscitation damage from oxygen.
These are examples of narrative fallacy that were compounded by trusting surrogate end points.
So which drug was best at preventing SCA?
Right up until they stopped the study, the doctors believed that all of them were preventing SCA.
As it turns out, post-MI PVCs do not cause SCA. Post-MI PVCs are indicators of a heart that is more likely to have one, or more, SCAs than hearts without post-MI PVCs.
Getting rid of the post-MI PVCs is no more effective at fixing the heart, than Botox is at making the patient younger. They just make things look better.
Post-MI PVCs are bad and making them go away is good. We are becoming more and more tolerant of PVCs and the patients with post-MI PVCs are not dropping like flies.
In hypertensive crisis, we must lower the pressure right away before we get to the ED. A more controlled lowering of the blood pressure in the ED seems to avoid making the patient worse.
Oxygen. More is better. Perhaps oxygen should be treated as if it is a drug, since oxygen is a drug. Perhaps we should figure out when to give a lot of oxygen, when to give a little oxygen, and when to withhold oxygen.
In CAST the patients receiving the study drugs encainide and flecainide were more than 3 times as likely to die as the patients receiving placebo. These life saving drugs were more than three times as likely to kill the patient.
Three times as deadly as what?
Three times as deadly as placebo.
The title as the most effective life saving drug on the planet, in this case, went to the placebo.
CAST was a study that showed how the top experts, the highest in the hierarchy, can be so sure that they are saving lives that they end up causing more harm than benefit. The greater harm was due to the life saving treatments the experts were promoting.
After the fact, there was a lot of concern about how the experts could have been so wrong. The reality was that these experts didn’t understand the pathophysiology as well as they thought they did.
But why did people listen?
Seeing is deceiving. No more PVCs. What more do you need to know?
–
Narrative Fallacy –
How did this happen? – Research
C A S T and Narrative Fallacy comment from Shaggy
Some Research Podcasting Comments
Shaggy Comments on Some Research Podcasting Comments.
Spine Immobilization in Penetrating Trauma: More Harm Than Good?
EMS EdUCast – Journal Club 2: Episode 43
Education Problems, Autism, and Vaccines
–
Footnotes:
–
[1] Mortality and morbidity in patients receiving encainide, flecainide, or placebo. The Cardiac Arrhythmia Suppression Trial.
Echt DS, Liebson PR, Mitchell LB, Peters RW, Obias-Manno D, Barker AH, Arensberg D, Baker A, Friedman L, Greene HL, et al.
N Engl J Med. 1991 Mar 21;324(12):781-8.
PMID: 1900101 [PubMed – indexed for MEDLINE]
Free Full Text Article from N Engl J Med with links to Free Full Text PDF download
CONCLUSIONS. There was an excess of deaths due to arrhythmia and deaths due to shock after acute recurrent myocardial infarction in patients treated with encainide or flecainide. Nonlethal events, however, were equally distributed between the active-drug and placebo groups. The mechanisms underlying the excess mortality during treatment with encainide or flecainide remain unknown.
–
[2] Medications for Arrest Rhythms
2005 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care
Part 7.2: Management of Cardiac Arrest
Free Full Text Article from Circulation with links to Free Full Text PDF download
To date no placebo-controlled trials have shown that administration of any vasopressor agent at any stage during management of pulseless VT, VF, PEA, or asystole increases the rate of neurologically intact survival to hospital discharge. There is evidence, however, that the use of vasopressor agents favors initial ROSC.
–
[3] Should a moratorium be placed on sublingual nifedipine capsules given for hypertensive emergencies and pseudoemergencies?
Grossman E, Messerli FH, Grodzicki T, Kowey P.
JAMA. 1996 Oct 23-30;276(16):1328-31. Review.
PMID: 8861992 [PubMed – indexed for MEDLINE]
Over the past 2 decades, nifedipine in the form of capsules has become widely popular in the treatment of hypertensive emergencies. . . . Given the seriousness of the reported adverse events and the lack of any clinical documentation attesting to a benefit, the use of nifedipine capsules for hypertensive emergencies and pseudoemergencies should be abandoned.
–
[4] The Oxygen Myth?
Bryan E. Bledsoe, DO, FACEP
JEMS.com Another Perspective
2009 Mar 5
Article
The effects of aging are often due to oxidative stress. Also, some diseases such as atherosclerosis, Alzheimer’s disease, Parkinson’s disease, and others have been linked to oxidative stress and free radical induction. Thus, the evolving thought is that, in some conditions, high concentrations of oxygen can be harmful.
.



[…] CAST and Narrative Fallacy […]