
There are several news articles today criticizing a study because the patients might be deprived of a drug that has not been adequately studied in humans. This criticism is coming from journalists – the people who publicized the fraudulent vaccines research by Andrew Wakefield, who was trying to sell his competing vaccine and was being paid to produce negative research by lawyers suing the vaccine companies.[1]
The real controversy is that this untested drug became the standard of care with no evidence that it improves outcomes that matter.
Is it controversial to give a placebo, rather than a drug not yet adequately tested in humans?
No.
We are not informing patients that there is no evidence that the standard treatment is effective. We are not obtaining consent to give the unproven drug – epinephrine (Adrenaline in Commonwealth countries). How are the ethics different when we substitute a placebo for a mystery medicine?
What is less ethical than continuing the tradition of giving an inadequately studied drug to people who cannot consent to treatment?
Are we depriving patients of effective medicine or are we depriving them of witchcraft?
If you think that epinephrine is effective medicine at improving survival to discharge, provide the evidence and stop this study. The reason the study is being done is that evidence of benefit does not exist.
Click on image to make it larger.[2] The studies are in the footnotes.[3],[4],[5],[6],[7],[8],[9],[10]
Is Adrenaline beneficial in cardiac arrest?
Probably, but only for some patients and we do not know which patients benefit.
Is Adrenaline harmful in cardiac arrest?
Probably, but only for some patients and we do not know which patients are harmed.
What is the right dose of Adrenaline in cardiac arrest?
Pick a number – any number. We do not know the right dose.
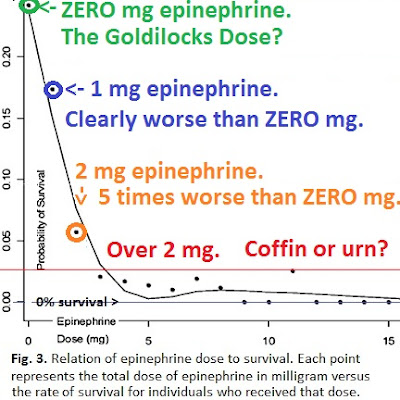
Even the patients who only received the minimum dose – 1 mg – had worse outcomes.[11]
Wrong timing? Wrong dose? Wrong drug?
We do not know.
We have used this untested treatment for half a century and not bothered to find out if it works. A recent study shows that epinephrine produces worse outcomes when given by EMS later,[12] but that does not mean that the outcomes are good when epinephrine is given early. The study had no placebo group, so like a study comparing different doses of cyanide, just because one dose is not as bad as another dose, the results do not suggest that cyanide is beneficial.
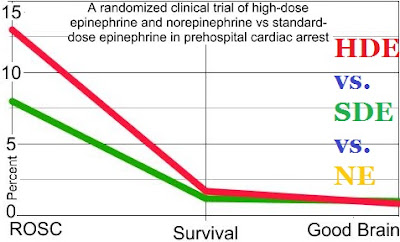
This is comparing three different treatments HDE (High-Dose Epinephrine), SDE (Standard-Dose Epinephrine), and NE (NorEpinephrine). The lines for the HDE and NE are so close to each other, that you may not be able to see the gold line.[13] Other studies produce similar results.[3],[14],[15],[16],[17] Only one study showed better ROSC with standard dose epinephrine.[18]
Epinephrine does produce more ROSC (Return Of Spontaneous Circulation – at least a temporary pulse) than placebo, but high dose epinephrine produces even more ROSC than standard dose epinephrine, so why do we give the standard dose that only produces middling ROSC?
Is ROSC the goal? No.
For the guidelines (ACLS and ILCOR), ROSC is the basis for giving standard dose epinephrine, but it would make more sense to give high dose epinephrine if the goal is ROSC. More ROSC, but no more survivors leaving the hospital. If all we want is put the patient in a coma long enough to run up a big hospital bill, then the drugs are great.
If we want people to leave the hospital alive, then We Do Not Know What Works.
The guidelines are based on wishful thinking and rationalization. They are not based on improved survival. A lot of research is cited (hundreds of papers), but the research does not show improved survival with any drug(s).
Will the guidelines be revised to remove epinephrine? Maybe.
The exciting development is that these data create equipoise about the current standard of resuscitation care. The best available observational evidence indicates that epinephrine may be harmful to patients during cardiac arrest, and there are plausible biological reasons to support this observation. However, observational studies cannot establish causal relationships in the way that randomized trials can.[19]
Some cocktails have produced better results than epinephrine in tiny studies. It is too probably too early to tell if these are just statistical aberrations. I will write about them later.
Continued in Does a Placebo vs. Adrenaline Study Deprive Patients of Necessary Care According to the Resuscitation Guidelines?
–
Footnotes:
–
[1] “Piltdown medicine” and Andrew Wakefield’s MMR vaccine fraud
Science-Based Medicine
Posted by David Gorski
January 6, 2011
Article
In a mere decade and a half, several decades of progress in controlling this scourge had been unravelled like a thread hanging off a cheap dress, all thanks to Andrew Wakefield and scandal mongers in the British press.
–
[2] Vasopressors in cardiac arrest: a systematic review.
Larabee TM, Liu KY, Campbell JA, Little CM.
Resuscitation. 2012 Aug;83(8):932-9. Epub 2012 Mar 15.
PMID: 22425731 [PubMed – in process]
CONCLUSION: There are few studies that compare vasopressors to placebo in resuscitation from cardiac arrest. Epinephrine is associated with improvement in short term survival outcomes as compared to placebo, but no long-term survival benefit has been demonstrated. Vasopressin is equivalent for use as an initial vasopressor when compared to epinephrine during resuscitation from cardiac arrest. There is a short-term, but no long-term, survival benefit when using high dose vs. standard dose epinephrine during resuscitation from cardiac arrest. There are no alternative vasopressors that provide a long-term survival benefit when compared to epinephrine. There is limited data on the use of vasopressors in the pediatric population.
–
[3] High dose and standard dose adrenaline do not alter survival, compared with placebo, in cardiac arrest.
Woodhouse SP, Cox S, Boyd P, Case C, Weber M.
Resuscitation. 1995 Dec;30(3):243-9.
PMID: 8867714 [PubMed – indexed for MEDLINE]
–
[4] Adrenaline in out-of-hospital ventricular fibrillation. Does it make any difference?
Herlitz J, Ekström L, Wennerblom B, Axelsson A, Bång A, Holmberg S.
Resuscitation. 1995 Jun;29(3):195-201.
PMID: 7667549 [PubMed – indexed for MEDLINE]
–
[5] Survival outcomes with the introduction of intravenous epinephrine in the management of out-of-hospital cardiac arrest.
Ong ME, Tan EH, Ng FS, Panchalingham A, Lim SH, Manning PG, Ong VY, Lim SH, Yap S, Tham LP, Ng KS, Venkataraman A; Cardiac Arrest and Resuscitation Epidemiology Study Group.
Ann Emerg Med. 2007 Dec;50(6):635-42. Epub 2007 May 23.
PMID: 17509730 [PubMed – indexed for MEDLINE]
Free Full Text Download in PDF format from prdupl02.ynet.co.il
–
[6] Intravenous drug administration during out-of-hospital cardiac arrest: a randomized trial.
Olasveengen TM, Sunde K, Brunborg C, Thowsen J, Steen PA, Wik L.
JAMA. 2009 Nov 25;302(20):2222-9.
PMID: 19934423 [PubMed – indexed for MEDLINE]
–
[7] Outcome when adrenaline (epinephrine) was actually given vs. not given – post hoc analysis of a randomized clinical trial.
Olasveengen TM, Wik L, Sunde K, Steen PA.
Resuscitation. 2011 Nov 22. [Epub ahead of print]
PMID: 22115931 [PubMed – as supplied by publisher]
–
[8] Effect of adrenaline on survival in out-of-hospital cardiac arrest: A randomised double-blind placebo-controlled trial
Jacobs IG, Finn JC, Jelinek GA, Oxer HF, Thompson PL.
Resuscitation. 2011 Sep;82(9):1138-43. Epub 2011 Jul 2.
PMID: 21745533 [PubMed – in process]
Free Full Text PDF Download from semanticscholar.org
This study was designed as a multicentre trial involving five ambulance services in Australia and New Zealand and was accordingly powered to detect clinically important treatment effects. Despite having obtained approvals for the study from Institutional Ethics Committees, Crown Law and Guardianship Boards, the concerns of being involved in a trial in which the unproven “standard of care” was being withheld prevented four of the five ambulance services from participating.
In addition adverse press reports questioning the ethics of conducting this trial, which subsequently led to the involvement of politicians, further heightened these concerns. Despite the clearly demonstrated existence of clinical equipoise for adrenaline in cardiac arrest it remained impossible to change the decision not to participate.
–
[9] Prehospital epinephrine use and survival among patients with out-of-hospital cardiac arrest.
Hagihara A, Hasegawa M, Abe T, Nagata T, Wakata Y, Miyazaki S.
JAMA. 2012 Mar 21;307(11):1161-8. doi: 10.1001/jama.2012.294.
PMID: 22436956 [PubMed – indexed for MEDLINE]
–
[10] Impact of early intravenous epinephrine administration on outcomes following out-of-hospital cardiac arrest.
Hayashi Y, Iwami T, Kitamura T, Nishiuchi T, Kajino K, Sakai T, Nishiyama C, Nitta M, Hiraide A, Kai T.
Circ J. 2012;76(7):1639-45. Epub 2012 Apr 5.
PMID: 22481099 [PubMed – indexed for MEDLINE]
Free Full Text from Circulation Japan.
–
[11] Wide variability in drug use in out-of-hospital cardiac arrest: A report from the resuscitation outcomes consortium.
Glover BM, Brown SP, Morrison L, Davis D, Kudenchuk PJ, Van Ottingham L, Vaillancourt C, Cheskes S, Atkins DL, Dorian P; Resuscitation Outcomes Consortium Investigators.
Resuscitation. 2012 Nov;83(11):1324-30. doi: 10.1016/j.resuscitation.2012.07.008. Epub 2012 Jul 31.
PMID: 22858552 [PubMed – indexed for MEDLINE]
Free Full Text from PubMed Central.
–
[12] Time to administration of epinephrine and outcome after in-hospital cardiac arrest with non-shockable rhythms: retrospective analysis of large in-hospital data registry.
Donnino MW, Salciccioli JD, Howell MD, Cocchi MN, Giberson B, Berg K, Gautam S, Callaway C; American Heart Association’s Get With The Guidelines-Resuscitation Investigators.
BMJ. 2014 May 20;348:g3028. doi: 10.1136/bmj.g3028.
PMID: 24846323 [PubMed – in process]
–
[13] A randomized clinical trial of high-dose epinephrine and norepinephrine vs standard-dose epinephrine in prehospital cardiac arrest.
Callaham M, Madsen CD, Barton CW, Saunders CE, Pointer J.
JAMA. 1992 Nov 18;268(19):2667-72.
PMID: 1433686 [PubMed – indexed for MEDLINE]
–
[14] A comparison of standard-dose and high-dose epinephrine in cardiac arrest outside the hospital. The Multicenter High-Dose Epinephrine Study Group.
Brown CG, Martin DR, Pepe PE, Stueven H, Cummins RO, Gonzalez E, Jastremski M.
N Engl J Med. 1992 Oct 8;327(15):1051-5.
PMID: 1522841 [PubMed – indexed for MEDLINE]
–
[15] Standard doses versus repeated high doses of epinephrine in cardiac arrest outside the hospital.
Choux C, Gueugniaud PY, Barbieux A, Pham E, Lae C, Dubien PY, Petit P.
Resuscitation. 1995 Feb;29(1):3-9.
PMID: 7784720 [PubMed – indexed for MEDLINE]
–
[16] A comparison of repeated high doses and repeated standard doses of epinephrine for cardiac arrest outside the hospital. European Epinephrine Study Group.
Gueugniaud PY, Mols P, Goldstein P, Pham E, Dubien PY, Deweerdt C, Vergnion M, Petit P, Carli P.
N Engl J Med. 1998 Nov 26;339(22):1595-601.
PMID: 9828247 [PubMed – indexed for MEDLINE]
–
[17] High dose versus standard dose epinephrine in cardiac arrest – a meta-analysis.
Vandycke C, Martens P.
Resuscitation. 2000 Aug 1;45(3):161-6.
PMID: 10959014 [PubMed – indexed for MEDLINE]
–
[18] High-dose epinephrine in adult cardiac arrest.
Stiell IG, Hebert PC, Weitzman BN, Wells GA, Raman S, Stark RM, Higginson LA, Ahuja J, Dickinson GE.
N Engl J Med. 1992 Oct 8;327(15):1045-50.
PMID: 1522840 [PubMed – indexed for MEDLINE]
–
[19] Questioning the use of epinephrine to treat cardiac arrest.
Callaway CW.
JAMA. 2012 Mar 21;307(11):1198-200. doi: 10.1001/jama.2012.313. No abstract available.
PMID: 22436961 [PubMed – indexed for MEDLINE]
Link to a free 6 1/2 minute recording of an interview with Dr. Callaway about this paper.
On the right side of the page, to the right of the First Page Preview, is a section with the title Multimedia Related by Topic. Below that is Author Interview. Below that is some information about the edition, . . . , and below that is an embedded recording of the interview. Press on the arrow to play. That has the recording of the interview with Dr. Callaway.
The interview with Dr. Callaway is definitely worth listening to.
–
Larabee TM, Liu KY, Campbell JA, & Little CM (2012). Vasopressors in cardiac arrest: a systematic review. Resuscitation, 83 (8), 932-9 PMID: 22425731
–
Woodhouse SP, Cox S, Boyd P, Case C, & Weber M (1995). High dose and standard dose adrenaline do not alter survival, compared with placebo, in cardiac arrest. Resuscitation, 30 (3), 243-9 PMID: 8867714
–
Herlitz J, Ekström L, Wennerblom B, Axelsson A, Bång A, & Holmberg S (1995). Adrenaline in out-of-hospital ventricular fibrillation. Does it make any difference? Resuscitation, 29 (3), 195-201 PMID: 7667549
–
Ong ME, Tan EH, Ng FS, Panchalingham A, Lim SH, Manning PG, Ong VY, Lim SH, Yap S, Tham LP, Ng KS, Venkataraman A, & Cardiac Arrest and Resuscitation Epidemiology Study Group (2007). Survival outcomes with the introduction of intravenous epinephrine in the management of out-of-hospital cardiac arrest. Annals of emergency medicine, 50 (6), 635-42 PMID: 17509730
–
Olasveengen, T., Sunde, K., Brunborg, C., Thowsen, J., Steen, P., & Wik, L. (2009). Intravenous Drug Administration During Out-of-Hospital Cardiac Arrest: A Randomized Trial JAMA: The Journal of the American Medical Association, 302 (20), 2222-2229 DOI: 10.1001/jama.2009.1729
–
Olasveengen TM, Wik L, Sunde K, & Steen PA (2011). Outcome when adrenaline (epinephrine) was actually given vs. not given – post hoc analysis of a randomized clinical trial. Resuscitation PMID: 22115931
–
Jacobs IG, Finn JC, Jelinek GA, Oxer HF, & Thompson PL (2011). Effect of adrenaline on survival in out-of-hospital cardiac arrest: A randomised double-blind placebo-controlled trial. Resuscitation, 82 (9), 1138-43 PMID: 21745533
–
Hagihara A, Hasegawa M, Abe T, Nagata T, Wakata Y, & Miyazaki S (2012). Prehospital epinephrine use and survival among patients with out-of-hospital cardiac arrest. JAMA : the journal of the American Medical Association, 307 (11), 1161-8 PMID: 22436956
–
Hayashi Y, Iwami T, Kitamura T, Nishiuchi T, Kajino K, Sakai T, Nishiyama C, Nitta M, Hiraide A, & Kai T (2012). Impact of early intravenous epinephrine administration on outcomes following out-of-hospital cardiac arrest. Circulation journal : official journal of the Japanese Circulation Society, 76 (7), 1639-45 PMID: 22481099
–
Glover BM, Brown SP, Morrison L, Davis D, Kudenchuk PJ, Van Ottingham L, Vaillancourt C, Cheskes S, Atkins DL, Dorian P, & the Resuscitation Outcomes Consortium Investigators (2012). Wide variability in drug use in out-of-hospital cardiac arrest: A report from the resuscitation outcomes consortium. Resuscitation PMID: 22858552
–
Donnino, M., Salciccioli, J., Howell, M., Cocchi, M., Giberson, B., Berg, K., Gautam, S., Callaway, C., & , . (2014). Time to administration of epinephrine and outcome after in-hospital cardiac arrest with non-shockable rhythms: retrospective analysis of large in-hospital data registry BMJ, 348 (may20 2) DOI: 10.1136/bmj.g3028
–
Callaham M, Madsen CD, Barton CW, Saunders CE, & Pointer J (1992). A randomized clinical trial of high-dose epinephrine and norepinephrine vs standard-dose epinephrine in prehospital cardiac arrest. JAMA : the journal of the American Medical Association, 268 (19), 2667-72 PMID: 1433686
–
Brown CG, Martin DR, Pepe PE, Stueven H, Cummins RO, Gonzalez E, & Jastremski M (1992). A comparison of standard-dose and high-dose epinephrine in cardiac arrest outside the hospital. The Multicenter High-Dose Epinephrine Study Group. The New England journal of medicine, 327 (15), 1051-5 PMID: 1522841
–
Choux C, Gueugniaud PY, Barbieux A, Pham E, Lae C, Dubien PY, & Petit P (1995). Standard doses versus repeated high doses of epinephrine in cardiac arrest outside the hospital. Resuscitation, 29 (1), 3-9 PMID: 7784720
–
Gueugniaud PY, Mols P, Goldstein P, Pham E, Dubien PY, Deweerdt C, Vergnion M, Petit P, & Carli P (1998). A comparison of repeated high doses and repeated standard doses of epinephrine for cardiac arrest outside the hospital. European Epinephrine Study Group. The New England journal of medicine, 339 (22), 1595-601 PMID: 9828247
–
Vandycke C, & Martens P (2000). High dose versus standard dose epinephrine in cardiac arrest – a meta-analysis. Resuscitation, 45 (3), 161-6 PMID: 10959014
–
Stiell IG, Hebert PC, Weitzman BN, Wells GA, Raman S, Stark RM, Higginson LA, Ahuja J, & Dickinson GE (1992). High-dose epinephrine in adult cardiac arrest. The New England journal of medicine, 327 (15), 1045-50 PMID: 1522840
–
Callaway, C. (2012). Questioning the Use of Epinephrine to Treat Cardiac Arrest JAMA: The Journal of the American Medical Association, 307 (11) DOI: 10.1001/jama.2012.313
–
Edited 12-27-2018 to correct link to pdf of Jacobs study in footnote 8.
.



Pardon me for my density if this is noted somewhere, but I’m having trouble finding anything regarding the method used behind the survival probability vs. epinephrine dose graphic. Is there a possibility of the increased doses correlating with decreased survival due to increased down time? I.e, could the higher doses be from frequency of 1mg doses? For instance, 2mg+ total epinephrine SHOULD correlate with decreased survival due to a probable down time of 10+ minutes or more, when factoring in time between EMS activation and contact and IV/IO access, etc.
On a sidenote: I think your evidence-based (cliché, I know) approach to EMS is refreshing and wholly necessary. It makes things a lot easier when I can cite credible sources when I challenge many of the antiquated protocols and whatnot in my own system. So, in short, thanks!